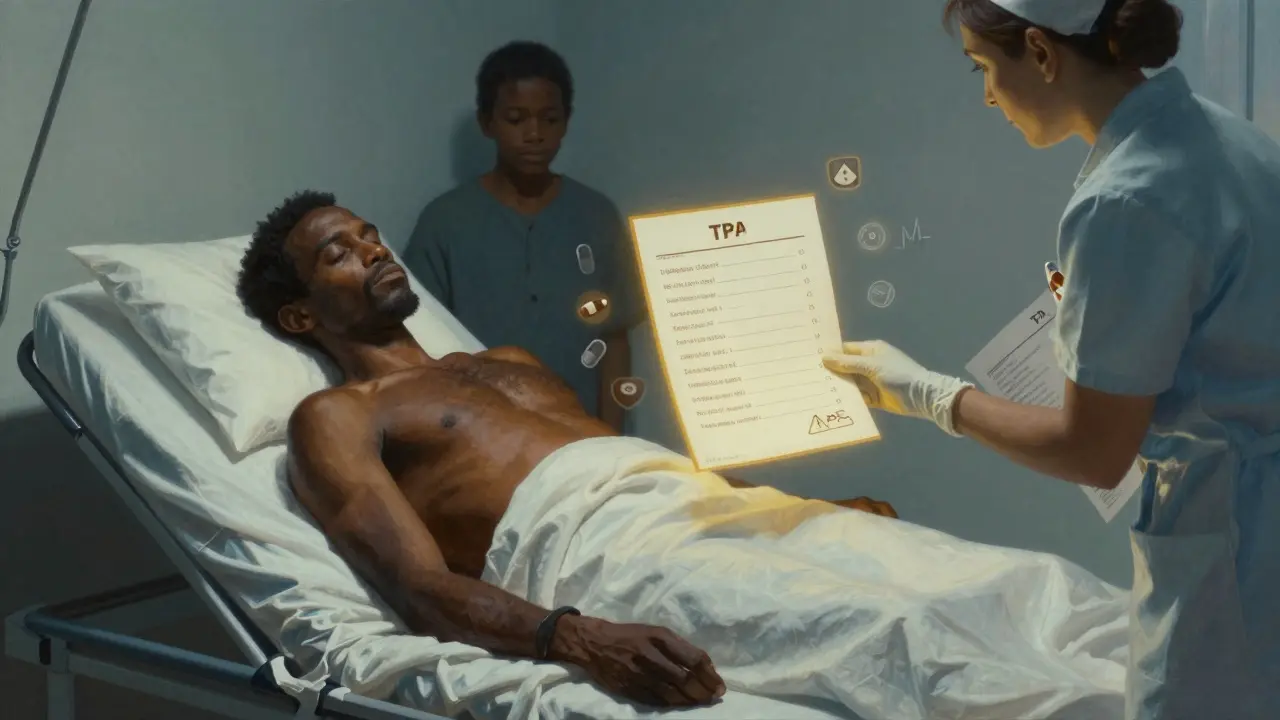
When you're traveling abroad and something goes wrong - a sudden allergic reaction, chest pain, or a fall - the last thing you want is to struggle to explain what pills you're taking. Emergency staff don't speak your language. You're scared. Your heart is racing. And in that moment, a simple piece of paper in the right language can mean the difference between life and death.
That’s why keeping a medication list in multiple languages isn’t just a good idea - it’s a necessity. It’s not about being prepared for a vacation. It’s about surviving an emergency when you can’t speak.
Why a multilingual medication list saves lives
Studies show that language barriers increase medication errors by up to 50% during emergency visits. In the U.S. alone, over 25 million people have limited English proficiency. Spanish, Chinese, Vietnamese, Arabic, and Tagalog are among the most common languages spoken at home. But most hospitals and clinics don’t have staff who speak all of them.
When a patient can’t explain their meds, doctors guess. They might give you a drug that interacts with something you’re already taking. They might miss a life-threatening allergy. Or worse - they might not realize you’re on blood thinners and accidentally perform a procedure that causes internal bleeding.
Research from the American Pharmacists Association found that patients who carried a multilingual medication list had emergency room visits that were, on average, 22 minutes shorter. That’s not just convenience - it’s critical. In a stroke or heart attack, every minute counts.
What to include on your list
A good multilingual medication list isn’t just a copy of your prescription bottle. It needs to be clear, complete, and easy for a stranger to understand. Here’s what you need to write down for each medication:
- Medication name - Use the brand name (e.g., Lipitor) and the generic name (e.g., atorvastatin). Some countries use different names.
- Dosage - How much you take (e.g., 10 mg, 500 mg).
- Frequency - When you take it (e.g., once daily, twice a day, as needed).
- Purpose - Why you take it (e.g., "for high blood pressure," "for diabetes," "for pain").
- Prescribing doctor - Their name and clinic/hospital.
- Start date - When you began taking it.
Don’t forget supplements, herbal remedies, or over-the-counter drugs. Many people take turmeric, ginkgo, or traditional Chinese herbs - but these can interact dangerously with prescription meds. Include them. If you’re unsure whether something counts, include it anyway.
Which languages should you use?
You don’t need to translate into 20 languages. Focus on the ones that matter to you.
Start with:
- Your native language
- English (if you’re traveling outside your home country)
- The language of the country you’re visiting
- Any language spoken by family members who might help in an emergency
For example, if you’re from Vietnam and traveling to France, you need Vietnamese, English, and French. If you’re from Nigeria and going to Germany, you need Hausa or Yoruba, English, and German.
According to the British Red Cross, the top 10 languages needed in European emergency rooms include Arabic, Urdu, Polish, Russian, Albanian, and Somali. If you’re planning to travel to places with large immigrant populations, check local health department reports - they often list the most common languages spoken in hospitals.
Where to get reliable multilingual templates
Don’t rely on Google Translate. Medical terms can be mistranslated. A phrase like "take with food" might become "take with dinner" - and that’s not the same thing.
Use these trusted sources:
- Tennessee Pharmacists Association (TPA) Universal Medication List - Available in 10 languages including Spanish, Chinese, Vietnamese, Korean, Arabic, Russian, Somali, Nepali, and French. It’s free to download as a PDF. The layout is simple and standardized across all versions.
- NPS MedicineWise app (Australia) - Works on iOS and Android. Lets you store your meds digitally, set reminders, and switch between 11 languages. Even if you’re not in Australia, you can use the app. It’s free and works globally.
- MedlinePlus - Run by the U.S. National Library of Medicine. Offers medication guides in over 40 languages. You can print out their templates or use them as a reference.
- British Red Cross Emergency Multilingual Phrasebook - Not a medication list, but it has key phrases like "I am taking," "I am allergic to," and "This medicine is for my heart." Great to carry alongside your list.
Pro tip: Download PDFs of these templates onto your phone. Save them in a folder labeled "Emergency Meds." Also print two copies - one to keep in your wallet, one in your luggage.

How to translate accurately
If you’re translating your own list, here’s how to avoid mistakes:
- Use a professional translator - not a friend or family member. Even if they speak the language, they might not know medical terms.
- Ask your pharmacist. Many pharmacies now offer free translation services for patients with limited English.
- Use the templates from trusted sources above. They’ve been reviewed by medical professionals and linguists.
- Check for dialects. Mandarin and Cantonese are both Chinese, but they use different characters. If you’re from Hong Kong, use Traditional Chinese. If you’re from mainland China, use Simplified.
One real-life example: A woman from Laos was brought to an ER in the U.S. with chest pain. She had a list in Lao, but the translator used Thai terms - which are similar but not the same. The doctor misread the dosage. She ended up in intensive care. A correct translation would have prevented it.
Keep it updated
Medication lists become useless if they’re outdated. Every time your doctor changes your prescription - adds a new pill, stops one, changes the dose - update your list.
Set a reminder: Every three months, check your list. Update it. Print a new copy. Delete the old one from your phone.
Studies show that 78% of medication errors happen during transitions of care - like going from hospital to home, or switching doctors. If your list is outdated, it’s worse than having no list at all.
Digital vs. paper
Which is better? Both.
Digital lists (like the MedicineWise app) are great because you can update them instantly, add photos of your pills, and share them with family. But if your phone dies, or you lose it, you’re back to square one.
Paper lists are simple, reliable, and don’t need batteries. Carry one in your wallet. Keep another in your travel bag. Use a clear plastic sleeve to protect it from spills.
Best practice: Have both. Store the digital version on your phone. Carry the printed version with you at all times.
What to do in an emergency
If you’re in an emergency and can’t speak:
- Hand the staff your printed medication list immediately - don’t wait to be asked.
- Point to the medication you’re taking right now. Say "this one" if you can.
- If you have a medical alert bracelet, point to it too.
- Ask for an interpreter. Most hospitals are legally required to provide one.
Don’t assume they’ll ask for it. Most ER staff are overwhelmed. They won’t think to ask about your meds unless you give them the tool to help.
Common mistakes to avoid
- Using only one language - even if you’re fluent in English. What if you’re unconscious?
- Writing "vitamins" instead of listing each one. "Vitamin D 1000 IU" is specific. "Vitamins" is not.
- Forgetting herbal supplements. Many people take ginger for nausea or ashwagandha for stress - these can cause dangerous interactions.
- Not checking the translation. A mistranslated "as needed" could become "only when you feel like it." That’s not the same.
- Leaving it at home. If you’re traveling, carry it. Always.
Real stories
A man from Somalia was brought to an ER in Minnesota after collapsing. He had a printed TPA list in Somali and English. The ER team recognized his medication for high blood pressure immediately. They avoided giving him a drug that would’ve caused a dangerous drop in blood pressure. He survived.
A grandmother in California had a stroke. Her granddaughter handed the nurses a medication list in Vietnamese. The nurses saw she was on warfarin - a blood thinner - and immediately ordered a CT scan. Without the list, they might have given her clot-busting drugs and caused a fatal bleed.
These aren’t rare cases. They happen every day.
What’s next?
The U.S. and other countries are moving toward digital health records that automatically translate medication lists. In 2024, the CDC added Amharic, Hmong, and Karen to its multilingual resources. Google now shows translated medication info directly in search results for over 30 languages.
But until those systems are perfect - and they won’t be for years - the simplest tool still works best: a printed list, in the right languages, carried with you.
Don’t wait for an emergency to make one. Do it now. While you’re still healthy. While you’re still calm. While you have time to get it right.
Can I use Google Translate to make my medication list?
No. Google Translate often gets medical terms wrong. For example, "take with food" might translate as "take with lunch," which isn’t accurate. Some drugs need to be taken with any meal, not just breakfast. Always use a trusted template from a medical source like the Tennessee Pharmacists Association or NPS MedicineWise. If you need help translating, ask your pharmacist - many offer free translation services.
What if my language isn’t on the list?
If your language isn’t available in official templates, find a professional translator who specializes in medical documents. Contact your local hospital’s language services department - they often have lists of certified translators. You can also ask your doctor’s office. Make sure the translation includes all five key elements: name, dosage, frequency, purpose, and prescribing doctor. Don’t skip any.
Should I include over-the-counter drugs and supplements?
Yes. Many serious drug interactions happen with supplements. For example, garlic, ginkgo, or St. John’s wort can interfere with blood thinners. Even common painkillers like ibuprofen can be dangerous if you’re on kidney or heart meds. List everything - even if you think it’s "just a vitamin." Better safe than sorry.
How often should I update my list?
Update it every time your doctor changes your meds - whether they add, remove, or adjust a dose. Then print a new copy. At minimum, review it every three months. Outdated lists are dangerous. One study found that 78% of medication errors happen during transitions of care - like moving from hospital to home - when lists aren’t current.
Is the MedicineWise app safe to use outside Australia?
Yes. The app works anywhere in the world. It doesn’t rely on Australian health systems - it’s just a tool for storing your personal medication list. You can switch between 11 languages, set reminders, and even add photos of your pills. It’s free, secure, and doesn’t require an account. Many travelers use it to manage meds while abroad.





Bhaskar Anand
This is complete nonsense. In India, we don't need fancy multilingual lists. If you're abroad and can't speak English, you're already in trouble. No one cares about your Hindi or Tamil meds. Just carry your prescription and shut up. Stop overcomplicating life.
William James
I love this post. Seriously. I used to think this was overkill until my dad had a stroke in Japan and we had no idea what he was on. The printed list in English and Japanese? Saved his life. No drama. No guesswork. Just facts. Everyone should do this. It's not about being fancy. It's about being smart.
David McKie
Oh please. Another feel-good piece of performative safety. You think a piece of paper is going to save someone in a chaotic ER? Hospitals are understaffed, overwhelmed, and frankly, incompetent. You're giving people false hope. And don't even get me started on the 'trusted sources'-NPS MedicineWise? That's an Australian app. Who cares? This is a Band-Aid on a hemorrhage.
Southern Indiana Paleontology Institute
I'm from Indiana and I gotta say-this is the dumbest thing I've read all week. Why do you need 5 languages? Just write it in English. If you're abroad and can't read English, maybe you shouldn't be traveling. Also, 'herbal remedies'? That's just witchcraft. People die from this stuff. You're not a doctor. Stop pretending you are.
lela izzani
I'm a nurse in Chicago. I see this every day. Last month, a woman came in unconscious. No ID. No info. Then her daughter handed me a laminated card in Spanish and English. We found she was on warfarin. We avoided a stroke. It took 3 minutes. That’s 3 minutes she didn’t bleed out. This isn’t theoretical. It’s real. Do it.
Spenser Bickett
So let me get this straight. You want me to carry a pamphlet like I'm going to a foreign country and not a hospital? Next you'll tell me to wear a tinfoil hat and carry a crystal for 'energy alignment'. We're not in a sci-fi movie. If you're that scared, don't leave the house.
Christopher Wiedenhaupt
I appreciate the thoroughness of this guide. The structure is logical. The sources cited are credible. The emphasis on professional translation over Google Translate is especially important. I've seen too many cases where mistranslations led to adverse events. This is a well-researched and necessary resource.
John Smith
Multilingual lists? How quaint. The real problem is that our healthcare system is broken. You think a piece of paper fixes systemic language gaps? Please. The ER staff don't speak your language? Hire interpreters. Fix the system. Don't put the burden on the patient to carry a dictionary.
Shalini Gautam
I'm from Delhi and I travel to Dubai every year. I have my list in Hindi, English, and Arabic. My mom uses it too. It's printed on cardstock, laminated, and in my purse. I also have it on my phone. Simple. No drama. And yes, I include my turmeric capsules. One time, the pharmacist in Dubai asked me about it. He said it was interacting with my BP meds. Saved me from a hospital visit. This isn't just advice. It's survival.
Nandini Wagh
Oh wow. So now we're supposed to be medical translators for our own bodies? What's next? A QR code that plays a 3-minute video of us explaining our meds? This is what happens when people think empathy is a checklist.
Holley T
I've been reading this whole thing and I'm just... baffled. You're telling people to carry a paper list? In 2024? Why not just use a blockchain-based decentralized health ID with AI-powered real-time translation? That's what we should be building. Not paper. Not apps. Not translations. We need infrastructure. This is like recommending a horse and cart because the Tesla has a flat tire. It's not just outdated-it's actively harmful. We're clinging to analog solutions while the world moves on. And you're celebrating it like it's a breakthrough. It's not. It's a failure of imagination.
Ashley Johnson
I know this sounds crazy but I think the CDC is secretly using these lists to track people. They're collecting data on your meds, your language, your ethnicity. Then they're feeding it to Big Pharma. That's why they're pushing these templates. You think they care about you? They want to know who's on blood thinners so they can sell you more drugs. Don't be fooled. I saw a guy in the ER get a bill for $12,000 after they 'discovered' his supplements. Coincidence? I don't think so.
tia novialiswati
This is so helpful! 💕 I made mine last month and put it in my wallet with a photo of my pills. My sister cried when she saw it. We all need to do this. You're not being dramatic-you're being responsible. ❤️
Alfred Noble
I'm a retired paramedic. I've seen it all. The paper list? Yeah, it helps. But the real hero is the person who carries it. Not the paper. Not the app. The person who thought ahead. That's the quiet kind of bravery nobody talks about. Keep it simple. Keep it close. And for god's sake, update it. Outdated info kills faster than silence.